Tag Archives: Myocardial infarction
It’s never too soon
No-one ever thinks they will get impacted by Heart Disease. We live in blissful ignorance until one day, if they’re lucky, they get a “warning”, a “wake up call”.
Many aren’t that lucky.
In 2010, over 45,000 people under the age of 75 died of Heart Disease in the UK.
That’s certainly how it was for me. I was bullet-proof. Until I wasn’t.
Once a week, the Cardiac Rehabilitation sessions have an hour of education. I consider this the “Community Service” session, where I do the time for the crimes I’ve committed in the past. The same crimes as many people, but I got caught!
This morning we talked about the anatomy of the heart. We covered much of the same ground when I was in hospital (see “You are what you eat“). I’ve had 5 weeks to think about what I could or should have asked… our questions and concerns were on a completely different level back then.
What I learnt today…
- The reason why atheroma builds up in some arteries and not others is not known
- The build up can start early (in your teenage years)
- Once it’s there, there’s nothing that can be done to reverse the build-up of atheroma
- It can only get worse, not better (drugs can help reduce the associated risk, but don’t reverse the build-up either)
- The only way of assessing the build-up is by performing an angiogram which itself carries a risk of 1 death in 1,000 from Heart Attack or Stroke
- Prevention is the best strategy
- It’s too late for me to adopt this strategy (but I knew that already!)
What’s happened to me could happen to anyone. It’s never too soon to become aware. Never too soon to take evasive action.
I know it doesn’t seem real, particularly if you’re young, fit and healthy. It won’t. Until it is. And then it’s too late.

Emotional Wreck (FD +3)
Another average night’s sleep (at best). I woke early, and put on my iPod so I could close my eyes and listen to some relaxing music… “Dignity” (Deacon Blue) got to me.
I’ve always liked the song, the sentiment and the story, but my reaction is a bit much. Fortunately it’s early. There are no witnesses. No-one will ever know!
I decided to take control. I set up the Blog. I’ve done it before. It’s straightforward. It only takes a few minutes for the basics. Immediately it helped me get my head together… do I want to be a “heart attack victim” or “heart attack survivor”? Even in my current emotional state, it’s a no brainer! (Incidentally, try searching the 2 phrases on Google… I got 2.1m hits for “victim” versus only 111k for “survivor”. What does that say?)
It was still early. Going home today. I needed to rest. How about a film to take my mind off things…
 In retrospect, “Saving Private Ryan” wasn’t the best selection ever. In fact, I may start a petition to have it removed from the options in the cardiac wards.
In retrospect, “Saving Private Ryan” wasn’t the best selection ever. In fact, I may start a petition to have it removed from the options in the cardiac wards.
After the first 27 minutes I was wrecked. Wrung out. I hung on for the uplifting finish, but even that’s traumatic and laden with sadness.
Next time it’s Disney all the way!
Should I stay or should I go? (FD +2)
I was at the point where I wanted to go home, return to some sort of normality, but slightly concerned it may be a little early. What would happen if something went wrong? Will I be tempted to do too much? Will we all cope without the nurses?
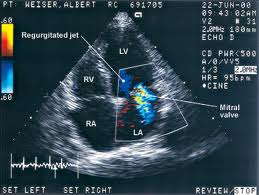
 The one test I still had to have was the Heart Echo – critical as it’d provide an insight on how much permanent damage had been done to my heart.
The one test I still had to have was the Heart Echo – critical as it’d provide an insight on how much permanent damage had been done to my heart.
Fortunately I didn’t have to wait too long… my number came up first, just as my toast and marmalade was being polished off.
It was strange being able to see my “broken” heart working away inside me. I knew they were measuring different dimensions, capacities, throughput rates, pressures, etc. I could see everything on the monitor, but I had absolutely no idea what anything meant.
 I couldn’t stop thinking of people I’ve known at work that were “OK” at their jobs, or new to their roles, learning as they went.
I couldn’t stop thinking of people I’ve known at work that were “OK” at their jobs, or new to their roles, learning as they went.
It felt to me like the Sonographer had quite an important role for me at that point in time. I hoped she was good!
I didn’t have to wait long for the results…
The diagnosis was that the permanent damage was low to intermediate, “to be expected” apparently. This meant that I would not be able to drive for 4 weeks (there was an outside chance it could have been only 1) and, if I wanted, I could leave hospital today… but leaving tomorrow was fine too. My call…
Right… decisions… (I’m getting out of practice!)
- If I can, I will stay an extra night. This will give us all time to get our heads around the idea of having a cardiac patient in our house
- Given it’s 4 weeks till I can drive, I may as well tie-in my return to work. It had been bothering me. Initially, the tendency was towards “the sooner the better”, but I don’t have to rush and I want to be able to do a proper job when I return. I could start after a couple of weeks, but who knows what shape I’d be in. Being able to commit to a date is important. 14th July it is!
Having made the decision, I’m told they need the bed.
“We need the bed. Could you leave today?”
“Oh, OK.”
“This afternoon would be good.”
“Oh, OK.”
I texted Louise. Much excitement (panic?!). Arrangements to be made (school pick-up, snacks, etc.). As soon as everything had been sorted…
“It’s alright. I’ve spoken to the doctor. You are staying another night.”
“Oh, OK”
Thank goodness for SMS and understanding relatives!
You are what you eat (FD +1)
The Rehab Nurse reminded me of Gillian McKeith (“You are what you eat”). Friendly while being knowledgeable and firm. She had the difficult task of running (Louise & I) through what had happened, why, and helping us to start thinking about “What next?”.
We already knew I scored quite high on the heart attack risk factors:
- Smoking – I wasn’t smoking but had been up until about 9 months ago
- High cholesterol – A family favourite
- High Blood Pressure – Certainly stress has been a feature of my work life for years
- Being overweight / obese – Certainly room for improvement
- Lack of exercise – Check
- Alcohol – Check
- Male – Check
See the full list: www.nhs.uk/conditions/heart-attack/pages/causes.aspx
Addressing any of these, together with the medication would help me prevent recurrence.
The most difficult one for me is work (which leads to Stress, which leads to High Blood Pressure). I can see me making major changes to other areas of my life, but I need time to get my head around what changes I might be able to make at work. Hopefully addressing some of the other factors will make me fit enough to do what I do, and help change my approach / attitude to it. Let’s see. (The Rehab Nurse sees “one or two like me” every week… I’m sure we’ll come back to this!).
The only “Life Decision” we were ready for related to our holiday. The ladies had unselfishly decided that two weeks in the summer heat of Florida, chasing thrills and spills at the Theme Parks and bargains at the Mall probably wasn’t the best recuperation for me. Swimming with the dolphins would have to wait. It would be cancelled immediately… thank goodness we took the insurance!
As far as physical activity is concerned, I could start walking gently as soon as I’m free from the monitor. As soon as I leave hospital I should start walking 5 mins, twice a day, and then add a minute on each day, slowly building strength and stamina. We were also informed that we could re-start “bedroom activities” after a week… this information was as useful as being told at Ante-Natal classes not to have any “intimate relations” after the water’s have broken… yeh, right!
Father’s Day (Approx. 00.30)
“Louise…”
“Louise!”
Deep breath… as loud as I could manage…
“LOUISE!!!”
“What?”
“I think I’m having a heart attack.”
“Don’t be so stupid, you’re not having a heart attack!”
I’ve done some research subsequently and it turns out that many, if not most, female nurses in Aberdeen would have responded to their partners in exactly the same way. Similar conversations:
(While cooking) Male: “I think I’m having a heart attack”
Female: “Are you hungry?”
M: “Yes”
F: “You’re not having a heart attack!”
M: “I think I’m having a heart attack”
F: “Do you have shooting pains down both arms?”
M: “No”
F: “You’re not having a heart attack!”
M: “I think I’m having a heart attack”
F: “Did you put the bins out?”
…
You get the idea!
The bottom line is, it’s difficult to get your head around the fact that your partner might be having a heart attack.
We had gone to bed together at about 11pm. Tired. We were looking forward to Father’s Day Lunch and a bag of balls on the driving range at Donald Trump’s new course near Aberdeen.
I guess it must have been around midnight when I awoke feeling a little strange – some tightness in my chest that seemed to come and go (lessen at least) as I raised my left arm above my head. I had cooked my “Killer Chilli” (poor name in hindsight!) for dinner, so indigestion was the obvious initial diagnosis.
After a few minutes I got up and went to the bathroom. I started to feel worse fast. More tight. More discomfort. An unfamiliar feeling. I laid on the floor and called for help.
“I really think I am having a heart attack. Please, call an ambulance.”
“You’re not having a heart attack… let me check…”
There then followed a serious of questions to compare my symptoms with those of a “typical” heart attack.
“Please, just call an ambulance.”
“I’ll call NHS 24, they’ll know what to do…”
Within 5 minutes, an ambulance was dispatched.
I couldn’t get comfortable. I would even go so far as to say I was in “extreme discomfort” (although I’m still struggling to translate this onto a “marks of out 10 pain scale”).
If I was having a heart attack, we knew “time means muscle” (“minutes mean myocardium”). We knew aspirin was a good idea… we didn’t have any aspirin. (Doh!)
Thankfully, the ambulance arrived quickly.
The Paramedics were calm, methodical and professional. They were everything you’d want in my position. They performed a variety of tests (including the 1st of many ECGs), and administered some basic medicines (to slow this, reduce that, etc.) before packing me off.
Finally I was dispatched into the balmy heat of an Aberdeenshire night (I shivered like I’ve shivered before) and on into the ambulance for some oxygen and morphine (“to take the edge off”).


